F.A.Q.
-
Cataract Surgery
With the formation of a cataract activities like reading, bowling, or driving can be difficult. Fortunately, vision can be restored quickly, allowing the patient to return home within a few hours. With new advances in cataract surgery noticed vision improvement begins almost immediately and an eye patch isn't even needed.
What is a cataract?

A cataract is the clouding of the lens of eye. Normally, light passes through the clear lens and is focused onto the retina. However, as a result of the natural aging process, the lens gradually becomes cloudy. The cataract or cloudy lens blocks the passage of light through the eye and causes distorted or blurred vision.Restoring Vision
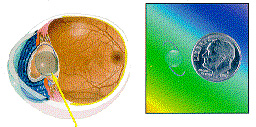 Once a cataract has formed, the most effective way to restore vision is to remove the cloudy cataract and replace it with a plastic lens implant (Intraocular lens or IOL).
Once a cataract has formed, the most effective way to restore vision is to remove the cloudy cataract and replace it with a plastic lens implant (Intraocular lens or IOL).
With recent advances in cataract surgery equipment and techniques, vision can be restored safer and faster, allowing patients to resume normal activities within hours after surgery (some activities may be limited during healing). Using these state of the art technics, cataract surgery has a success rate greater than 98%.Topical or No Needle Anesthesia
Previously cataract surgery was performed under general anesthesia requiring patients to stay in the hospital. Later advances used a local anesthesia (retrobulbar or peribulbar blocks) where a needle stick is made, penetrating to just behind the eyeball where the anesthetic is injected. Although this procedure allows patients to return home the same day and is safer than using general anesthesia, it is not entirely free of risk Today, with recent advances in cataract surgery anesthesia, topical anesthetics are used. A patient may be given an IV sedative to help them relax and to keep them comfortable during the procedure. Next, the eye is anesthetized with eye drops instead of a needle injection.Advantages of Topical Anesthesia
- Faster with greater patient comfort
- No patient anxiety over receiving a deep injection next to the eyeball.
- Visual recovery begins immediately since the eye muscles aren't paralyzed as with local block anesthesia.
- Eliminates potential complications such as perforation of the eye, hemorrhage or damage to the optic nerve.
- Removes the chance for a relatively dangerous anesthesia induced allergic reaction.
- Eliminates potential for post operative headaches caused by conventional blocks.
- Eliminates need for an eye patch.
No-stitch, Self Sealing Incision Surgery
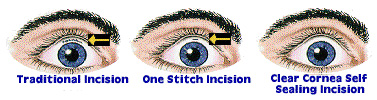
Ultrasound technology (phacoemulsification or "phaco") is often used to remove a cataract. With "phaco", the probe is inserted through a small 1/8 opening (instead of a relatively wide incision) created with a specific self sealing technique.
The new techniques place the incision into the cornea (clear part of the eye that covers the iris or colored portion of the eye) just next to the schlera (white part of the eye).Advantages of the No-Stitch, Clear Corneal Incision
- No placement or removal of sutures
- May be performed under local or topical anesthesia
- Requires No Patch when combined with topical anesthetics
- It is a bloodless incision
- Reduces postoperative restrictions
- Improves postoperative vision and minimizes postoperative astigmatism
Ultrasound is used to gently break-up or emulsify) the cloudy lens into tiny pieces which can be removed through the tip of the "phaco" probe instead of a wide incision. A special lens can then be implanted through the smaller incisionAfter surgery
Many patients are pleased to find that after topical, clear corneal cataract surgery their vision improvement begins almost immediately and they return home within a few hours after the procedure. Patients may find their vision better than ever; however, some will need to wear glasses for reading and other activities following the procedure. During the initial healing period there may be a few limitations on strenuous activities . However, most people find they are able to return to a normal lifestyle immediately, plus start doing things poor cataract vision had restricted them from doing in the past."Secondary" Cataracts
During cataract surgery a clear capsule surrounding the cataract is left in place to support the lens implant. In some cases this capsule may turn cloudy months or years after surgery creating a "secondary" cataract. If this occurs an outpatient laser procedure will quickly restore good vision.
-
Is Topical Anesthesia, No-stitch, No-patch Cataract Surgery For Everyone?
In most cases the topical anesthesia, no-stitch, no-patch techniques are preferred, however some patients, because of their eye structure, health or other factors, may not be good candidates for the new techniques. In these cases, patients can have traditional surgery and expect to do well. A complete eye examination and consultation with Dr. Mendoza is necessary to determine each individuals specific needs and potential for improved vision.
Sight loss can be prevented
Loss of sight from the cataracts is usually preventable. With modern technology, cataracts can be removed and good vision restored when a person feels the loss of vision is great enough to interfere with daily activities. If you are experiencing the symptoms of cataracts or other vision problems, you should obtain a complete eye examination.
Strabismus
Strabismus is one of the most common pediatric eye problems, as approximately 4% of children are born with the condition. However, strabismus can also affect adults. Strabismus is a condition in which the eyes are misaligned or point in different directions. The eyes do not work or turn together in a parallel fashion. If the eyes turn in, the person is "cross eyed". If the eyes are turned out, the person is "wall eyed". The eyes may also turn up or down.
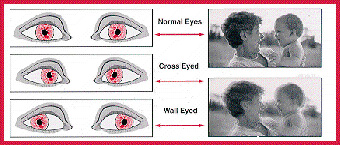
What causes strabismus?
Strabismus is caused by an eye muscle imbalance. A misplaced muscle or weak muscle causes one eye to turn in, out, up or down. Although the exact reason for the defect in the eye muscles is unknown, strabismus is frequently hereditary in nature. Eye movement is controlled by three pairs of muscles which are attached to the outside of each eyeball. One set moves the eye right or left, while the other two sets move the eye up and down and control tilting movements. For normal vision, both eyes must line up together and focus on a single object. Each pair of muscles must be balanced and working together with the corresponding muscles of the other eye. When the muscles do not work together, strabismus occurs.
-
How does strabismus affect vision?
In normal vision, both eyes look at the same object at the same time. Each eye then sends a picture to the brain, and these two pictures are blended into one three-dimensional image. Strabismus prevents both eyes from focusing on one object simultaneously. As a result, two conflicting images are sent to the brain. The image sent by the straight or dominant eye is clear, but the message sent by the misaligned or weaker eye is blurry. The brain is unable to blend the two images into one picture. A child quickly and unconsciously learns to ignore or suppress the image seen by the weaker eye. The stronger eye takes over, while the misaligned eye becomes lazy from lack of use. If left uncorrected, the weak or lazy eye will eventually develop amblyopia, or a loss of vision. An adult who develops strabismus will usually experience double vision. The adult brain is already trained to receive images from both eyes and is unable to ignore the image from the misaligned eye.
-
What are the symptoms of strabismus??
Strabismus is often difficult to detect. The condition may be present at birth or may develop two to three years later. With strabismus, the eyes may appear abnormal all the time or only when the child is ill, tired or concentrating on near objects. Besides a misaligned eye, other symptoms of strabismus include turning or tilting of the head, squinting of one or both eyes, getting too close to objects and not seeing as clearly as others. Infants often appear to have strabismus when they do not. Because the bridge of an infant's nose is flat and underdeveloped, the extra skin on either side of the nose may cover up the inner white portion of the eye. This makes the eyes appear to be crossed when they are not. As the child grows, the nose narrows and the eyes appear normal. Unfortunately, a child cannot outgrow true strabismus. Left untreated, strabismus can lead to a permanent loss of vision. Therefore, early eye examinations are extremely important in the detection of strabismus, as well as other vision problems.
-
How is strabismus diagnosed?
A complete eye examination is necessary to diagnose strabismus. After the medical history of the child and family is gathered, the child's eyes are tested. Vision may be tested with the E test in which the child is asked to point in the same direction as the "fingers" of a capital E on the eye chart. A series of progressively smaller E's is used to determine how well the child can see. With very young children, a picture chart or the ability to follow a small object may be used as a substitute for the E test. External eye muscles are tested by examining how each eye moves. The eyes are also checked for any signs of disease with an ophthalmoscope, a special lighted instrument for examining the back of the eyes.
-
How is strabismus treated?
Prompt treatment of strabismus is necessary to preserve good vision. If strabismus is not corrected by the age of six, the child will probably have poor vision for the rest of his life. Any straightening of the eyes after that time will usually only improve the child's physical appearance, not his vision. The goal of strabismus treatment is to restore good vision first, then to straighten the eyes, and finally, if possible, to make the eyes work together. A combination of corrective glasses, patching, eye drops, eye exercises, and surgery is used to treat strabismus.
Children who are farsighted may cross their eyes when looking at close objects. In such cases, glasses are often prescribed to help straighten a child's eyes. Sometimes eye glasses which correct farsightedness will successfully straighten the eyes. However, additional treatment is often necessary. Patching the good eye or using medicated eye drops to temporarily blur vision in the good eye may be used to encourage use of the misaligned eye. When the vision of the straight eye is blocked, the lazy eye is forced to work. The earlier patching is started, the more effective it will be. The later it is started, the longer it will take to correct strabismus.
Eye exercises may also be helpful in some cases of strabismus. The exercises are designed to help the eyes move together and to focus on the same object at the same time. If nonsurgical methods fail to correct strabismus, surgery to adjust the muscle tension in one or both eyes may be necessary. A tiny incision is made in the outer covering of the eye where the muscles are attached. The muscles are either strengthened or weakened to achieve the correct tension. The incision is closed with tiny stitches which are absorbed by the eye tissue. The patient is usually able to return to normal activities a couple of days after surgery.
Although usually only one surgery is necessary to correct strabismus, more than one operation is sometimes needed. In addition, glasses and patching may still be required after surgery to complete the treatment. If a treatment program is started early and followed carefully, strabismus can be corrected. Both the parent and child must stick to the treatment plan to ensure permanent straightening of the eyes and good vision. -
Prevention is the best medicine
Eye examinations, during infancy and preschool years, are extremely important in preventing vision loss from strabismus. If strabismus is not detected until after a child has entered school it may be impossible to reverse any sight loss which has occurred. Eye examinations are especially important if there is any history of strabismus in the family. When strabismus is diagnosed, prompt treatment is necessary to prevent permanent vision loss.
If your child is experiencing the symptoms of strabismus or has not had his eyes checked, he should have a complete eye examination.
